Patient Centered Approach: EMU's simulation activity at St. Joseph Mercy Hospital shows the power of integrated care
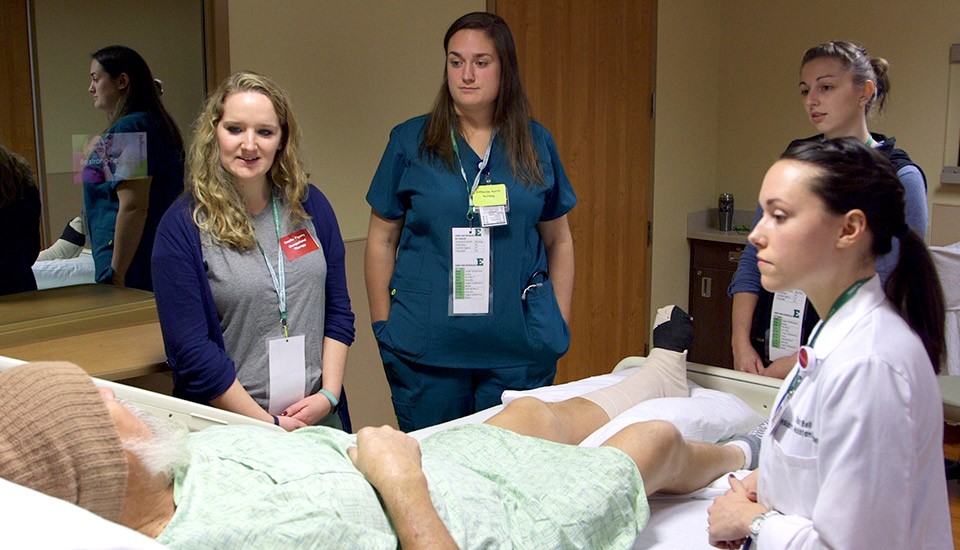
“Can I get a whiskey?”
The patient was neither cooperative nor very responsive.
He was a homeless man, an alcoholic who lived in a local park and had suffered frostbite, forcing the amputation of his foot, an outcome he had trouble understanding.
A team of three professionals—a dietitian, a nurse and a physician assistant—attempted to communicate and draw him out while assembling a plan to discharge him.
“We’re definitely here to help you,” the nurse said reassuringly. “We’re trying to make it so you can go home again.”
The patient tried to get up out of bed, which at that point would have been disastrous, given the need to first learn to walk on his newly amputated foot. The nurse quickly moved to gently but firmly block his attempt.
The helpful trio seemed young, and for good reason. They were students in graduate health-based programs at Eastern Michigan University, part of more than 50 soon-to-be professionals participating in a day of scenario practice and review last fall at the Patient Simulation Facility at nearby St. Joseph Mercy Hospital.
The day’s program, which combined students from a variety of health programs that also included orthotics and prosthetics, occupational therapy and social work, is part of a powerful emphasis and culture at the EMU College of Health and Human Services (CHHS) on interprofessional education (IPE)—the idea that patients benefit most from integrated care that blends the efforts of professionals from various areas.
“Patient and client needs demand that professionals from many different disciplines work together to provide the best care possible,” says Christine Karshin, associate dean of the college. “Simulation-based education, used in a collaborative practice, is of great value for learners outside their own disciplines. It better prepares students to meet the complexities of today's health care workplace.”
Indeed, a 2015 national report on malpractice risks in communications found that communications breakdowns figured in 30 percent of all malpractice claims filed between 2009 and 2013. Further, 37 percent of all high-severity injury cases (including death) involved a communication failure," the report said.
After undertaking the scenario, students reviewed their interactions on video and critiqued their performance along with an observing faculty member.
“I felt like the education just was not going to happen,” said the nursing student, noting that the simulated patient, a St. Joe’s retiree who worked in finance, excelled at playing the role of disoriented and frustrated patient. “I did not expect the patient to be that disruptive.”
After reviewing the video of their first scenario in small groups, students and faculty gathered together in a classroom to share impressions and insights. Professors Linda Myler and Kathy Seurynck, co-directors of the nursing simulation labs at EMU and organizers of the day’s program along with Jacob Lindquist, a professor of orthotics and prosthetics, led the discussion.
They noted that the simulated patients had been instructed to give in a little bit to the students, but then become disruptive in some fashion.
“What do you do when your plan goes (awry)?” they asked the students, adding that a takeaway from the exercise is that you need to be prepared for anything.
Students said they appreciate the college’s focus on IPE, with the bonus of bringing it to life in simulation facilities at St. Joe’s and EMU.
“I have always been an advocate for IPE since beginning my college education here at EMU,” said Dean Kot, who’s in the physician assistant program. “I enjoyed learning about the other career fields the CHHS offers and seeing them in action, even though it was a simulation.
“Each career field brought something else necessary to properly provide the patient with the care they need. This IPE event goes to emphasize the importance of a team-based approach and collaboration among each profession when working in healthcare.”
EMU has undertaken such efforts with the help of a $500,000 estate gift from Donald F.N. Brown, which helped the college establish an Interprofessional Faculty Scholars Conference and other educational activities.
Later in the day, students underwent a second simulation with their same patient. The priority for the homeless man was again to focus on a discharge plan. The students wanted to ensure the man could walk and would be safe when he returned to his “home.” A social worker joined the team.
“Do you have any family?” the students asked.
“She dead now,” the patient said of his mother, pausing for a second.
“Maybe that’s when I started drinking,” he added in a flat voice.
Vicki Washington, an instructor and lead faculty for psychiatric mental health nursing at EMU, watched the video with the students and seized on the remark – a crucial and teachable moment.
She said that further discussion could deepen understanding of the patient’s family history and influences, offering clues on how to help him going forward.
“That must have made you sad...” would be a prompt and engaging response to such a revealing admission, Washington told the students.
“That’s just a huge door opener,” she said.
Watch a video about the interprofessional education simulation at St. Joe's.
January 24, 2018
Written by:
Geoff Larcom
Media Contact:
Geoff Larcom
glarcom@emich.edu
734-487-4400
More Stories
EMU Honors Crochet and Knitting Club ties the community together through acts of service.

Southeast Michigan Stewardship Coalition at Eastern Michigan University appoints new leadership.




